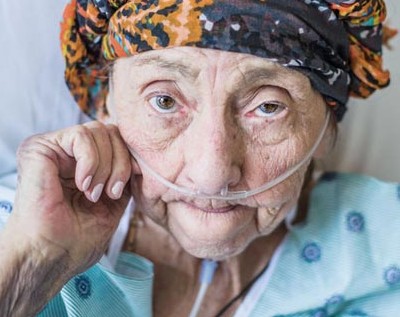
Hospice Admission Guidelines for Patients with Sepsis
Download a PDF of these guidelines.
Are you a patient, family member, or caregiver? Learn about how VITAS can help patients with end-stage sepsis.
By Joseph Shega, MD, Chief Medical Officer, VITAS Healthcare
The development of sepsis is associated with a very high in-hospital mortality. In fact, 1 (or more) in 3 hospital deaths are sepsis-related.1
Sepsis is one of the most serious conditions in the United States, with approximately 250,000 annual deaths. The estimated annual cost of sepsis readmissions is >$3.5 billion.2

Additionally, post-acute care use and hospital readmissions are common after sepsis. The increased readmission risk after sepsis was observed regardless of sepsis severity and was associated with adverse readmission outcomes.3
Sepsis 30-day readmissions are twice as likely to die or enroll into hospice compared to non-sepsis readmission.
Despite this, hospice is inadequately utilized for sepsis patients. In one study, 40% of sepsis deaths met hospice eligibility guidelines at the time of hospital admission.4
Any patient with advanced illness and a clinical complication of sepsis is a candidate for a goals-of-care discussion and the consideration of hospice services.
Clinical Progression of Sepsis
The clinical course of sepsis can be divided into pre-sepsis, sepsis and post-sepsis, with patients generally following a trajectory based on underlying health status.
Important determinants of status pre-sepsis include:
- Nutritional, functional and cognitive status
- Symptom burden in conjunction with:
- Medical factors (multi-morbidity and advanced illness)
- Contextual factors (healthcare utilization and social determinants of health)
- Pathogenic factors (virulence, load and antibiotic susceptibility)
Sepsis-related determinants include clinical manifestations plus some degree of system dysregulation. Clinical manifestations:
- Respiratory failure
- Circulatory shock
- Renal injury
- Delirium
- Metabolic changes
- Coagulopathy
- Liver injury
- Increased lactate
The most common advanced illnesses associated with sepsis-related hospital deaths include:
- Metastatic cancer
- NYHA class III/IV heart failure
- Advanced lung disease (defined as SOB at rest or with minimal exertion, with or without oxygen)
- Dementia with any difficulty in ADLs
The more clinical factors or organ dysfunction present, the higher the in-hospital mortality due to sepsis. Clinical complications include:
- Vasopressor use
- Mechanical ventilation
- Hyperlactatemia
- Acute kidney injury
- Hepatic injury
- Thrombocytopenia
Hospice Eligibility
Sepsis-related complications, particularly organ dysfunction, should trigger goals of care conversations, especially when the patient has an end-stage condition such as cancer (solid tumor or hematologic), heart disease, lung disease or dementia.
Patients with functional and cognitive impairments pre-sepsis are significantly more likely to die after hospital discharge than those patients who are functionally and cognitively intact—and should be referred to hospice.5
Patients who survive hospital-incurred sepsis often develop decrements in health status along with disease exacerbation such as impaired cardiac or lung function, refractory delirium/cognitive impairment, or dysphagia. As noted above, ED utilization and hospital readmission are common upon hospital discharge.
It is incumbent upon the hospital to delineate the most appropriate post-acute care site: skilled nursing, home health or hospice. Those patients eligible for hospice have an underlying advanced illness or, prior to sepsis, had an underlying physical disability or cognitive impairment.
Hospital Inpatient
- Hospice eligible, not previously identified
- Cancer-solid tumor and hematologic
- Heart disease
- Lung disease
- Dementia
- Clinical complications of sepsis
- Vasopressor use
- Mechanical ventilation
- Hyperlactatemia
- Acute kidney injury
- Hepatic injury
- Thrombocytopenia
At Hospital Discharge
- Hospice eligible, not previously identified
- Cancer-solid tumor and hematologic
- Heart disease
- Lung disease
- Dementia
- Pre hospital functional ability
- Physical impairment
- 1 of 6 ADL or 1 of 5 IADL
- Cognitive status
- Any degree of dementia
- Physical impairment
VITAS provides these guidelines as a convenient tool. They do not take the place of a physician's professional judgment.
1Centers for Disease Control and Prevention Data Reports. Available at: https://www.cdc.gov/sepsis/datareports/index.html
2Gadre, SK et al. Epidemiology and Predictors of 30-Day Readmission in Patients With Sepsis. CHEST 2019; 155(3):483-490
3Jones TK, et al. “Post-Acute Care Use and Hospital Readmission after Sepsis.” Ann Am Thorac Soc 2015 (12); 904–913
4Rhee C., et al. “Prevalence, Underlying Causes and Preventability of Sepsis-Associated Mortality in US Acute Care Hospitals.” JAMA Network Open. 2019;2(2):e187571
5Iwashyna TJ, et al. “Long-term Cognitive Impairment and Functional Disability Among Survivors of Severe Sepsis.” JAMA 2010;304(16):1787-1794]