How to Pay for Hospice Care (Medicare and Other Options)
Get the Guide: The Medicare Hospice Benefit
Does Medicare Cover Hospice?
Most hospice patients are eligible for the Medicare Hospice Benefit, which covers up to 100% of hospice services.
There is no reason to defer hospice care due to financial concerns. The Medicare Hospice Benefit is an inclusive benefit, in which all services that are related to the terminal illness are covered up to 100 percent by Medicare Part A. Care that is unrelated to the terminal illness continues to be covered by Medicare Parts A and B, with all normal rules applicable (e.g., co-payments, coverage guidelines, and deductibles).
What is Covered Under the Medicare Hospice Benefit?
Medicare Hospice Benefit coverage includes everything involved in hospice care, from visits by a nurse, physician, and other healthcare professionals, to therapy, medication, and supplies. Here is the complete list of services:
- An interdisciplinary team of hospice professionals
- Home medical equipment
- Medication
- Respite care
- Continuous care
- Inpatient care
- Routine home care
- Bereavement support
What Is Not Covered Under the Medicare Hospice Benefit?
While most hospice care is covered under the Medicare Hospice Benefit, it does not include the following items:
- Curative treatment, including any prescription drugs related to curative treatment.
- Emergency department care not related to the patient’s terminal diagnosis or not arranged by their hospice provider.
- Costs associated with room fees or rent for assisted living facilities and nursing homes as well as food. This includes mortgages or rent and food for patients living at home. (These items are covered for hospice patients who are experiencing a medical crisis due to symptom exacerbation and are staying in an inpatient unit (IPU) for the short term.)
How Long Will Medicare Pay for Hospice Care?
To be hospice-eligible, a patient must receive a diagnosis of a terminal illness from a physician, with a life expectancy of 6 months or less if the illness follows its normal course. However, sometimes patients live beyond this 6-month period.
If the hospice medical director/physician determines that the patient is no longer terminally ill with a prognosis of six months or less, they must discharge the patient from their care to the community.
If the patient’s terminal illness continues, they can be recertified for hospice. The Medicare Hospice Benefit covers an unlimited number of 90-90-60-day recertifications as long as the patient remains hospice eligible.
Patients’ physicians are involved in the recertification process as they continue to monitor patient status and prognosis.
Does Medicare Pay for Hospice Care at Home?
The Medicare Hospice Benefit covers end-of-life services related to a patient’s terminal diagnosis in whatever setting the patient calls home, whether that’s a traditional residence, an assisted living facility, or nursing home. Wherever hospice occurs, all services related to the terminal diagnosis are covered up to 100% by Medicare Part A.
If the patient’s symptoms cannot be managed by the routine level of hospice care, additional levels of service, such as 24/7 continuous care or inpatient hospice care, will also be financed through Medicare Part A at no additional expense to the patient or family.
Does Medicare Pay for Hospice in a Skilled Nursing Facility?
Yes, hospice services provided in a nursing facility are covered by Medicare. In a nursing home setting, hospice helps patients, families, and nursing home staff by providing end-of-life resources and support. The Medicare Hospice Benefit covers services, medications, supplies, and equipment that are related to life-limiting illness. It does not, however, cover expenses associated with room and board. These skilled nursing facility room-and-board expenses are often covered by Medicaid when the patient meets the state’s financial eligibility requirements.
The Medicare and Medicaid Hospice benefit also includes a provision for respite care and inpatient care, which can also be provided in a nursing facility for short stays. When the need for respite or inpatient hospice care is identified by the hospice team, the total costs associated with the care are covered under the hospice benefit.
How Do You Pay for Hospice Care Without Medicare?
For those not eligible for Medicare or Medicaid, payment for hospice can come from private insurance or an HMO, since these also include a hospice benefit.
Hospices employ financial specialists to help families who do not qualify for federal assistance and do not have insurance find available resources. The payment options for these families include self-pay and charitable organizations.
Facing a terminal illness brings with it many concerns. Paying for end-of-life care shouldn’t be one of them.
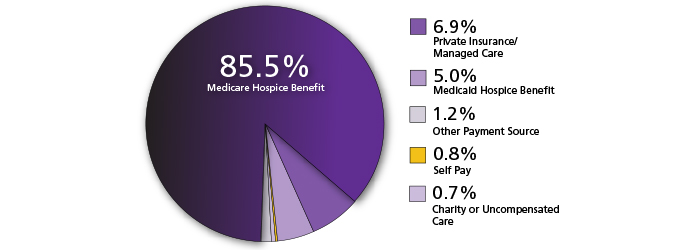
Source: NHPCO's Facts and Figures: Hospice Care in America