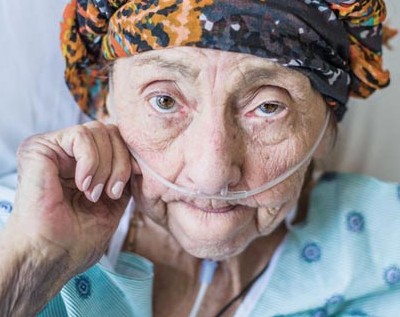
Legacy of Love: Families, Culture, and Advance Care Planning
Even in the best of times, family dynamics can be complicated. But when a family member is dying, relationships with loved ones can take on new significance and complexity.
In parent-child relationships, generational and cultural factors play a meaningful role in how the relationship evolves over time and how end-of-life care is handled.
When discussing end-of-life care, healthcare professionals can make the conversation more productive by being mindful of the cultural, generational, and personal beliefs involved.
When Death Is Culturally Taboo
In many cultures, deep respect is given to elders’ wishes even as they age. Difficult conversations about end-of-life care may never occur if an aging parent doesn’t bring it up, especially if talking about death is considered disrespectful, shameful, or taboo in their culture.
Asian Culture and End of Life
That is largely the case for Baby Boomer members of the Asian American community as they near the end of life, says Adam Kendall, MD, medical review physician for VITAS in Orange County, California.
For these patients, Dr. Kendall suggests speaking about hospice as a proactive, supportive benefit affecting the whole family, rather than as a medical specialty that anticipates near-death suffering. Patients may take more comfort from thinking of how they are caring for their children and their legacy than they would if the sole focus is their own need.
Related: 5 Best Practices for Providing Culturally Sensitive Care >
Hospice Opens up a Chance to Share
Even if parents have accepted their condition, children may be driven to seek care that seems to offer them unrealistic hope. They may underestimate the value of comfort and familiarity, which hospice relies on to support the entire family.
“Hospice gave us the courage and support to bring my dad home, and those five days changed me completely, forever.”-Birinder Marwah, MD, VITAS medical director
Birinder Marwah, MD, VITAS medical director in South Chicago, recalls trying to convince his father to move from New Delhi, India, to Chicago for care after a colon cancer diagnosis. Dr. Marwah thought his father could benefit from improved care and extra support; his father—a proud, retired Indian Army officer—simply preferred to face fate in the place he knew best.
When his father took a turn for the worse, Dr. Marwah brought both parents back to the US, and “in less than a day, the futility of what I had done became obvious. My father was dying and nothing could change that.”
Luckily, “hospice gave us the courage and support to bring my dad home, and those five days changed me completely, forever.” The Marwahs found time to share their feelings, their presence, and their love with one another. So moved was Dr. Marwah by his first hospice experience that the then-geriatrician redirected his career toward end-of-life care to help others discover the comfort and support it brought to his father and family.
“As I’ve become familiar with hospice...this aspect has become clearer to me: [aging parents] are very reluctant to share their unmet needs with their family, but once hospice is involved, the parents feel that they can bring these feelings out in the open.”
Dr. Illeana Leyva and Dr. Eric Shaban, VITAS regional medical directors, give a step-by-step demonstration of how to approach a goals-of-care conversation.
Coming to Consensus
Adult children and other family members bring their own fears and concerns about dying as they make decisions on their loved one’s behalf, says Jacob Huynh, MD, a VITAS physician in Orange County, California.
“Pause before providing unsolicited advice, especially prognostic advice.”-Adam Kendall, MD, VITAS medical review physician
In his primarily Vietnamese patient base, Dr. Huynh notices many families hesitate to wean their loved one from artificial nutrition, hydration, or antibiotics, even when doing so would contribute to a more comfortable death.
“Each patient and family has unique difficulties they have to overcome at the end of life, and we try to help them to successfully navigate this part of the journey,” he notes.
Dr. Huynh advises patients to “think more about what they want in advanced care, especially when they have multiple children who don’t always agree with the approach to care. That would make it easier when a life-threatening diagnosis arrives.”
Sunil Pandya, MD, associate medical director for VITAS in Naples, Florida, says even medical professionals can fail to find common ground in these contentious circumstances.
“My mother died in 2011 without hospice,” he says. “The family never had a good goals-of-care discussion, never had palliative care. My brothers and I were all well-educated—three of us in healthcare—but never came to a consensus on her care.”
Dr. Pandya attributes his choice to enter the hospice profession to this poignant end-of-life experience. A decade later, his father would die under his care at the VITAS inpatient unit in Collier County, Florida. The difference between the deaths was “night and day”: While his mother died in distress, alone in an ER without her family, his father was surrounded by loved ones who had time to physically, mentally, and spiritually prepare for the sad-but-unavoidable outcome.
“He couldn’t have had a more blessed ending to what was an eventuality that I couldn’t have changed,” Dr. Pandya says.
Leaving a Legacy
In some cultures, legacy and spirituality can intertwine. Tiffany Phuong, VITAS admission liaison in Orange County, California, says many older Vietnamese patients fear that dying at home could have a lasting impact on their successors.
“They’re afraid that if someone dies in the home, the spirit will remain in the home,” she says, “and some families may worry it will affect them when selling the home.”
These fears may be compounded by a patient’s or family’s concerns about those who are left behind, notes Dr. Kendall. Patients often find it easier to concentrate on someone who is not themselves, and “taking time to understand the family history or the virtues that help them be successful” is a key way to show respect to the patient and the family.
“Listen to understand who makes the life-changing decisions in the family and... pause before providing unsolicited advice, especially prognostic advice,” he says. “My own grandmother, a 106-year-old, at first struggled with incorporating a DNR and assisted home bathing. She now proudly speaks of how concerned she is of my aunt and uncle’s well-being.”
To Cultivate Trust, Start With a Conversation
When working with people of any cultural background, care professionals can cultivate trust and develop a deeper understanding of their patients’ needs by inquiring about relationship dynamics and family members’ concerns. Consider asking adult children about subjects their parent may find uncomfortable to discuss.
Goals-of-care conversations and advance care planning sessions offer natural starting points for discussing these topics, especially when family members attend.
Earn CE Credits
VITAS Healthcare offers free webinars hosted by experienced hospice professionals to educate clinicians on the benefits of hospice.
See Upcoming Webinars