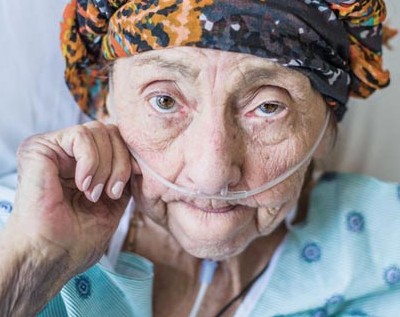
Pain’s Culturally Defined Role in Dying
Comfort and dignity are two of the primary goals of every hospice and palliative care plan. For most patients, pain management is integral to success.
Every patient experiences pain in their own way, so clinicians must consider unique physiological and psychosocial factors like the patient’s:
- Specific illness
- Physical state
- Cognitive and psychological state
- Drug allergies and interactions
- Personal tolerance for discomfort
Culture is a less-considered but crucial element of the individual pain experience. Culture can impact a patient's relationship with pain in surprising ways, from the sensation of pain itself to a patient’s willingness to communicate what they’re feeling.
Likewise, clinicians’ own beliefs and traditions can influence how they perceive, understand, and treat pain. Caring for patients whose cultural attitudes toward pain differ from one’s own presents a potential challenge—but also an opportunity for humility, learning, and growth.
“Cultural sensitivity is really important. People bring with them a whole story,” says Preeya Desh, MD, a hospital-based palliative care physician for VITAS Healthcare in West Palm Beach, Florida. “Coming at it with a lens that ‘this is how we do it here’ isn’t helpful for anyone. You’re talking two different languages.”
Cultural Influences on Pain
Hospice and palliative care clinicians know that the level of pain patients express does not always reflect what they're feeling. Some patients might not even recognize certain sensations as pain—or, at least, pain worthy of noting—based on their understanding of what’s “normal.” Culture can contribute to these expectations.
“’Take what comes’ is what we’ve been taught.”-Mythili Bharadwaj, MD, VITAS medical director
“In a lot of Asian cultures, the idea of suffering is accepted,” says Dr. Desh, who grew up in the US and attended medical school in India. “You’re asked to be a little more stoic, you’re expected to bear a certain level of pain.”
Deep-seated philosophical or religious beliefs also can explain certain cultural norms about pain and suffering. For instance, modern Christians, Jews, and Muslims have varying ideas about the origin and purpose of pain, but they generally believe in a common duty to relieve suffering where it exists. Some Hindus and Buddhists attribute an individual’s present suffering to karma—the accumulated moral value of a person’s actions across current and past incarnations—while others chalk it up to material attachment, or the will of a God or gods.
Resource: 5 Best Practices for Providing Culturally Sensitive Care >
Mythili Bharadwaj, MD, medical director for VITAS in St. Louis, Missouri, shares a cultural insight from her upbringing in India, a predominantly Hindu nation: Pain and misfortune in the present moment will pass, and those who are suffering often presume that “better things are coming.”
“It’s a culture we’ve been raised in and grown into,” she says. “’Take what comes’ is what we’ve been taught.”
Seeking Relief – or Not
A society’s material resources and medical infrastructure can influence cultural expectations about pain—and trust in pain management—as much as any belief system.
Munima Shaikh, MD, a palliative care physician for VITAS in Orlando, Florida, shares why Pakistani patients in the US might not seek out pain relief intuitively.
“We really don’t have much palliative care in Pakistan. Most patients who are seriously ill go home and die with their families,” says Dr. Shaikh. “We don’t have a lot of resources like pain medicine. Morphine is not widely available outside of major surgical hospitals.”
Related: How Diversity Influences Our Care for Patients >
In parts of the world where the hospice and palliative care disciplines are still developing, confusion and uncertainty may surround comfort-focused care, limiting usage by potentially eligible patients.
For example: “There’s a taboo associated with morphine [in Pakistan],” Dr. Shaikh says. “Pain medicine is associated with dying. That part is difficult to navigate, but once you explain it, it’s often fine.”
The Taboo of Death
Even veterans of comfort-focused care can feel uncomfortable discussing death, yet in certain cultures, the topic carries additional weight. Dr. Bharadwaj grew up in India, where death is an especially difficult subject. “Like in any close-knit society... it is a taboo to talk about dying,” she says. “This is where cultural sensitivity and cultural competence play a role.”
“Pause before providing unsolicited advice, including prognostic advice.”-Adam Kendall, MD, medical review physician
Cultural norms about elders can also complicate decisions about palliative care. Adam Kendall, MD, medical review physician in Orange County, California, has learned plenty about these subtle communication preferences from his experiences with Asian patients and families, and from his own Japanese American heritage.
“The Asian elder can delegate complex decision-making to a family member... or they may not wish to ever hear about the prognosis. They may feel it’s an act of shame to openly talk in their presence about the end of their life,” he says. “They may also prefer to focus on the aspects [of the end of life] that have to do with family wealth, or support of the next generation, and that may be foreign to the medical team.”
Dr. Kendall offers some advice worth considering before initiating a goals-of-care conversation, whether or not taboos are a concern:
“The best way to approach [cultural] barriers is to take the time to listen and understand who makes the life-changing decisions in the family,” he says, “and to pause before providing unsolicited advice, including prognostic advice.”
‘Clashing of Two Cultures’
Certain kinds of pain or distress may be treated as personal shortcomings among members of some immigrant communities, especially when stoicism and self-sufficiency are measures of success, notes Dr. Kendall.
He recalls encountering these perceptions both at home and within the medical community while seeking support for the depression faced by his late wife and fellow physician, Dr. Normy Chiou:
“She was a shining example of what some Asian Americans can overcome despite the clashing of two cultures. While she couldn’t share her illness very openly with family, she grew to understand the reasons underlying the high expectations and fear of shame. You strive to achieve or over-achieve to live up to the expectations of elders who brought you to the United States. There’s a sense of wanting to arrive at the success that took generations for your ancestors to reach.”
Overcoming with Culturally Sensitive Outreach
In the United States, the population of older (age 65+) people of color is growing rapidly, yet they are less likely than non-Hispanic whites to receive hospice care at the end of life, according to the National Hospice and Palliative Care Organization. Barriers to access are varied and complex: distrust of healthcare institutions, lack of local providers, and misunderstanding of or unfamiliarity with services represent just a few.
“You need to build that trust in the whole community.”-Patty Wu, MD, VITAS medical director
Providers can employ culturally sensitive outreach to overcome these issues, working with physicians and other trusted members of immigrant communities, minority religious organizations, and culturally specific medical associations to share information about the benefits of their services.
Tiffany Phuong is a VITAS representative on an all-Vietnamese team in Orange County, California. After speaking to a variety of groups and individuals in person, online, on television, and over the radio, she’s found that every educational opportunity has the potential to open doors to another.
“People come to one meeting and they think it’s very helpful, and then they invite me to their own group,” Tiffany says. “I want to help people to recognize how important that is. When I started 10 years ago, we hardly had Vietnamese patients. One positive experience brings others to us.”
People who feel their concerns are heard, and who understand how hospice and palliative care can address those concerns, are more willing to take a chance on an otherwise unfamiliar approach to care. Tiffany isn’t the only one to think so.
“The expectation [in some Asian cultures] is that we take care of our own, we don’t need someone coming into our house,” says Patty Wu, MD, medical director for VITAS in San Gabriel, California. “You need experience to take that leap of faith. You need to build that trust in the whole community, and that takes volume.”
‘We Need to Go in Without Bias’
According to Dr. Wu, the best hospice and palliative care advocates are patients and families who are willing to share their positive experiences within their own communities, using the familiar languages and terms of their cultural peers.
To produce these experiences, clinicians need to consider a person’s cultural perspective without relying on stereotypes or assumptions, approaching each patient first and foremost as an individual.
“There’s a broad conversation and exploration that has to happen [that involves] asking patients about their beliefs on an issue,” says Dr. Desh. “We need to go in without bias and paternalism. Suffering is a relative term, and as a physician, I need to honor that.”
Related Events

Tips for Effective Goals-of-Care Discussions
Conduct more effective goals-of-care discussions with your patients by using this conversation starter guide.
Download Now Clinicians: Receive Our Newsletters