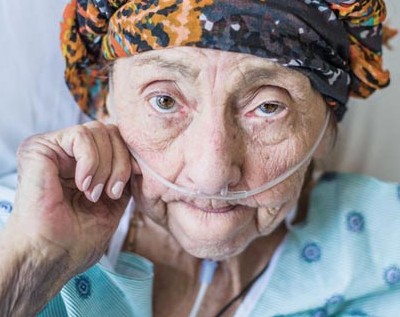
Lifting Quality of Life: How Hospice Delivers a Better Patient Care Experience
By Lauren Loftis, MD, Regional Medical Director, VITAS Healthcare
Many believe hospice is a brief window of care prior to death. That is the stigma. It is also a misconception. It misses how much life a patient can experience during hospice care, receiving pain and symptom management that allows them to live a quality of life that greatly surpasses constant hospitalizations and invasive procedures.

Louis Major, the subject of this article's case study, as a young man in Air Force uniform.
Louis Major is a powerful example of a hospice journey well lived. At 89 years old, Mr. Major is a decorated Air Force veteran who served as a fighter jet pilot for many years. In May 2023, he was unable to move his legs following a Pilates session. He went to the hospital and was admitted to the ICU. CT scans revealed advanced malignancy, and ED clinicians referred him to an oncologist. As his trusted primary care physician, he asked me what he should do. With a serious, life-limiting illness and terminal prognosis, I suggested he and his family discuss his options with VITAS team members.
“I don’t want to do anything that reduces my quality of life,” Mr. Major told me. “I want to continue doing Pilates and water aerobics and spend as much time as possible with my family. I don’t want to have invasive tests or procedures, and I don’t want to be in the hospital.”
Hospice honors these goals and values and provides evidence-based benefits, enabling Mr. Major to remain at home and participate in activities he enjoys with disease-directed medical care.
Supportive, Coordinated Care
With hospice, patients can stay in their preferred care setting, whether a private home, assisted living community, or nursing home. Like Mr. Major, data shows 80-90% of people prefer to be at home at the end of life.1
With VITAS, I can remain his attending physician. Referring physicians choose how involved they want to be in their patient’s care. While in hospice, Mr. Major also keeps his ties to the VA health system.
In addition, he receives visits from his hospice RN/case manager one to two times a week and has access to a home health aide, social worker, chaplain, and other team members who support him and his family. When he contracted COVID-19 over the winter, he stayed out the hospital—his expressed desire—with the help of respiratory therapy, oxygen, and consistent follow-up from VITAS clinicians.
Earlier Access: “If This Is the End, That’s Great”
Because Mr. Major decided to enter hospice immediately, he continues to remain active and leaves his home on excursions with his family. These activities keep him energized, even as his cancer progresses. Though he is weaker and has lost weight, his eyes still sparkle. Hospice has made all the difference.
The Medicare Hospice Benefit is an earned benefit for individuals facing serious illness with a prognosis of six months or less. This was Mr. Major’s prognosis, yet as of this writing, he continues to survive a year later. Like former President Jimmy Carter, Mr. Major continues to be hospice eligible because his prognosis remains six months or less if the illness runs its normal course. Research published in the Journal of Pain and Symptom Management found that Medicare beneficiaries who opted for hospice care lived an average of 29 days longer than similar patients who did not take advantage of hospice.2
Earlier access to hospice means a better quality of life for the patient, family, and caregiver, which is evident in Mr. Major’s case. He maintains control over his medical care in hospice, and his clinical team delivers the symptom management and pain control that stabilize him.
Most importantly, Mr. Major can spend quality time with his family. His veteran son and active-duty grandson were key participants in a pinning ceremony to honor his service. As his physician, I was able to attend along with my hospice care team members.
Referring to his overall experience, he told me: “If this is the end, that’s great.”
Levels of Care Focus on Need
Mr. Major receives a routine level of hospice care at home. Yet, if he needs a higher level of care, such as continuous home care, inpatient services, or inpatient respite care, to provide relief for his family caregivers, VITAS can provide it. Hospice is the only post-acute setting that can titrate to the level of care needed without changing the care setting.
With far more robust services than home health or palliative care, hospice also can offer complex symptom relief and high-acuity care. Hospice care costs are paid 100 percent by Medicare, Medicaid, and private insurance. Hospice is the only Medicare benefit that includes pharmaceuticals, medical equipment, 24/7 access to care, nursing, social services, chaplain visits, grief support following a death, and other appropriate services.
Cost-Effective Care That Increases Satisfaction
Greater utilization of hospice during the last six months of life is associated with increased satisfaction and quality of life, as Mr. Major’s example shows, while also reducing Medicare costs—$3.5 billion in savings in one year. On average, hospice episodes that fall into length-of-stay groupings of 15 days or longer are associated with lower total costs of care for hospice users than non-hospice users.3
By avoiding unhelpful treatments that increase costs without prolonging life, hospice patients experience fewer burdensome care transitions. Many families tell us, “We only wish we had chosen hospice earlier.”
For Mr. Major, making the hospice choice has given him the dignity of living the final stretch of life—his way. It has offered his family dedicated time with him. As his physician, his journey has been meaningful and uplifting, especially as I receive affirmation from his family that his care goals, wishes, and values are honored.
With increases in patient satisfaction and better pain control, reductions in hospital days, and reduced costs for healthcare systems, hospice may be the right option to suggest to your eligible patients.
1 Wang, et al. (2016). Transitions between healthcare settings of hospice enrollees at the end of life. Journal of the American Geriatrics Society, 64(2), 314-322.
2 Connor, S., et al. (2007). Comparing hospice and nonhospice patient survival among patients who die within a three-year window. Journal of Pain and Symptom Management, 33(3), 238-246.
3 NORC at the University of Chicago (2023). Value of Hospice in Medicare. Available at: https://www.nhpco.org/wp-content/uploads/Value_Hospice_in_Medicare.pdf
Earn CE Credits
VITAS Healthcare offers free webinars hosted by experienced hospice professionals to educate clinicians on the benefits of hospice.
See Upcoming Webinars