VITAS Patient-Centered Care: 4 Levels of Personalized Care
By Bryan Wysong, Senior Vice President, Operational Performance, VITAS Healthcare
Individuals facing serious illnesses may be approaching the final phase of their healthcare journey. Nevertheless, every patient deserves quality of life focused on what matters to them. For patients like these, VITAS® Healthcare offers four levels of care to ensure their final months, weeks, and days can be meaningful and fulfilling in their location of choice.
In addition to managing symptoms, hospice helps patients address spiritual needs as well as financial, practical, and relational matters. Making this part of their journey the best it can be—for both patients and their loved ones—drives my passion for hospice care.
Because VITAS elevates the level of care based on the patient’s need, we can reduce disruptive rehospitalizations and Emergency Department (ED) visits. Typically, patients receive clinical care in the comfort of their own home or other preferred setting. This eases their anxiety and offers loved ones’ peace of mind.
A Higher Level of Care: Four Levels Based on Patient Need
The Medicare Code of Federal Regulations (CFRs) requires hospices to provide four levels of care: hospice care at home, continuous hospice care, inpatient hospice care, and respite care.
| Four Levels of Care Mandated by the Medicare Hospice Benefit | |
|---|---|
| Home/Routine |
|
| Continuous Care (at VITAS, we call this Intensive Comfort Care*) |
|
| Inpatient |
|
| Respite |
|
While every Medicare-certified hospice provider must provide all four levels of care, in reality, not all hospices do. Based on data from the Centers for Medicare & Medicare Services (CMS), fewer than 28% of hospices reported providing continuous home care in 20221. Over the last four years, the number of hospice providers reporting no instances of continuous home care, inpatient respite care, or general inpatient care has steadily risen.
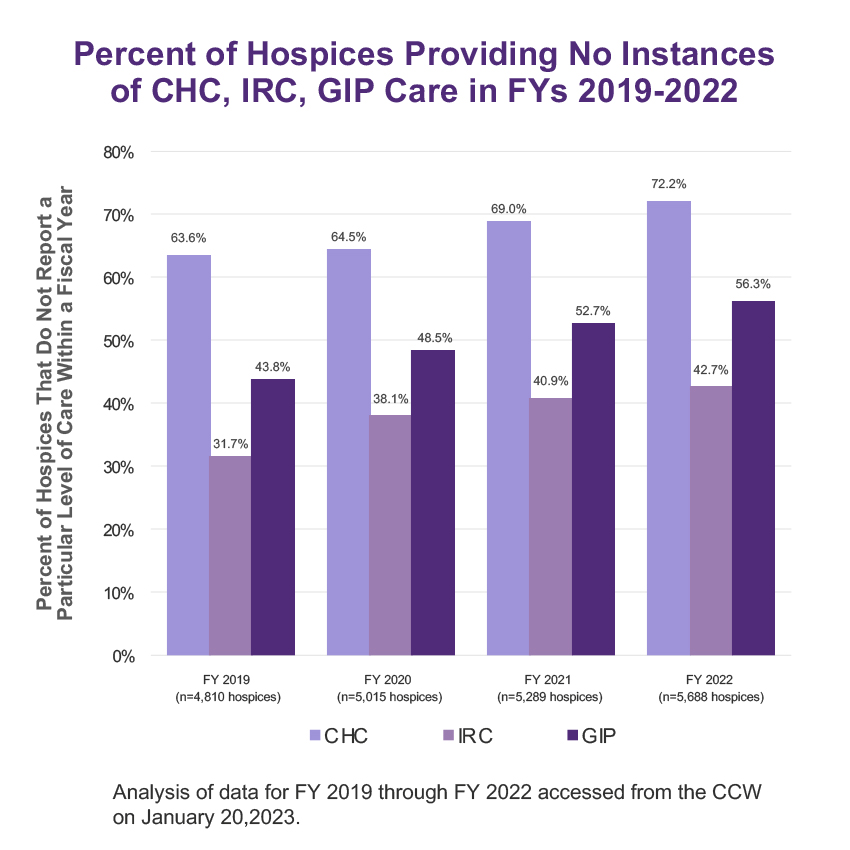
Selecting a hospice provider that does not provide high-acuity care can impact the patient and caregiver experience. According to CMS, “Hospices that are unable, or unwilling, to provide higher levels of care… may not adequately be able to care for patients who are in crisis or have symptoms that cannot be managed in the home, resulting in a worse outcome for the patient [and] a greater burden on caregivers which may worsen the quality of care at the end of life.”
Continuous Care vs. Inpatient Care
Continuous care and general inpatient care are similar. Both are designed for patients in a crisis who require a higher level of clinical assistance. Once a patient’s acute symptom exacerbation is resolved, patients are transitioned to a routine level of hospice care.
They differ in that general inpatient care must be provided in a skilled setting, such as a hospital, nursing home, or freestanding hospice facility.
Continuous home care, as its name suggests, offers this higher level of care in a patient's residential home or home-like environment, such as an assisted living community or nursing home. The VITAS care team provides shifts of care, which can be up to 24 hours a day.
Most commonly, LPNs care for patients along with HHAs. In addition, an RN will either visit in person daily or check in remotely. The patient benefits from the services of their entire interdisciplinary team, including an RN case manager, chaplain, social worker, and volunteers. At this higher level of care, their physician may also visit.
In 2022 alone, VITAS provided more than 1.3 million hours of continuous care shifts to its patients to manage acute symptoms in order to keep patients in location of choice.
Specialized Services Tailored to a Patient's Need
Along with expert clinical care, a personalized plan of care also includes specialty hospice services to ease symptom burden and provide an elevated patient care experience. To address specific patient needs, VITAS offers*:
- Respiratory therapy
- Physical therapy
- Occupational therapy
- Speech therapy
- Music therapy
- Dietary support
- Nutritional counseling
These services are arranged as needed by VITAS team members.
*Some services vary by program.
Expert Care Coordination Enhances Patient and Family Satisfaction
To ensure patients seamlessly transition to hospice care, VITAS coordinates care that aligns with the goals and wishes of the patient and their family. VITAS team members are responsible for:
- Sharing information with patients’ attending physicians
- Keeping patients and families informed of changes to the plan of care
- Managing timely transitions between care settings
- Providing the right care at the right time, in patients’ preferred setting
Our enhanced care coordination addresses the complexity of patients’ needs, including the provision of HME, supplies, and medications. VITAS has technology to facilitate coordination between hospice care teams and attending physicians, even for patients who see multiple healthcare professionals associated with several health systems.
Why Sooner Is Better for Hospice
Recent studies show hospice care improves patient outcomes—better symptom relief, goal attainment, and quality of life—with hospice stays over 30 days resulting in the highest quality of life outcomes.
Hospice offers multiple benefits to patients, families, and caregivers: increased satisfaction and quality of life, improved pain control, reduced physical and emotional distress, and reduced prolonged grief and other emotional distress.
1. Centers for Medicare & Medicaid Services (U.S.). (2023). Medicare Program; FY 2024 Hospice Wage Index and Payment Rule Update, Hospice Conditions of Participation Updates, Hospice Quality Reporting Program Requirements, and Hospice Certifying Physician Provider Enrollment Requirements. Dept. of Health and Human Services, Centers for Medicare & Medicaid Services.
Is your patient ready for hospice care?
Clinicians: Sign up for VITAS emails
Subscribe for end-of-life care news and free CE webinars.
Sign Up