More Than a Melody: Music Therapy Brings Out the Best in Patients, Caregivers
VITAS music therapist Peggy Grace strums a G major and lets the chord ring out.
“I’m in love–I’m all shook up,” she sings, and she’s not the only one. VITAS patient Patricia Browder, in her 80s and living with dementia, sings every word she remembers and mouths the handful she doesn’t.
Patricia sways, she claps, and her face makes it clear: She’s as happy as an Elvis superfan could be, barring a meeting with The King himself.
Both of Patricia’s private caregivers notice, and so does Peggy. This temporary boost to their patient’s mood is progress worth celebrating.
‘They Always Notice a Difference’
The heartwarming music therapy session, captured on video by one of Patricia’s caregivers, highlights the joyous power of this musical intervention. Music therapy isn’t right for every patient, but for many, it offers visible results surprisingly quickly.
“Whenever I go to meet Patricia, her caregivers will let me know whether she’s grumpy or down,” says Peggy, a music therapist for VITAS in Jacksonville, Florida. “They always notice a difference after her music therapy sessions. Her mood and her affect are brighter; she’s more pleasant and calmer.”
“It’s not just that her mood is lifted, but she’s also moving within her physical limitations.”-Music therapist Peggy Grace
For Peggy, that’s the goal for Patricia. While music therapy may look like a sing-along session to a casual observer–and sometimes, sing-alongs are involved–in actuality, it’s a hospice and palliative care intervention aligned to the diverse goals and wishes of each individual patient.
A music therapy care plan for a dementia patient such as Patricia, for instance, may focus on mood management and gentle sensory stimulation. For others, music therapy can be used to encourage reminiscing, prompt creativity, or promote movement in patients with limited mobility.
Peggy notes that some of her patients with dementia and Alzheimer’s are utterly unresponsive to external stimuli–until she begins playing their favorite tunes.
“Watching the video of Patricia, you’ll notice how she’s really engaged in the music. She’s having a great time clapping and singing,” Peggy says. “It’s not just that her mood is lifted, but she’s also moving within her physical limitations, which has an improved overall effect on her well-being.”
More Than Playing and Singing
Music therapy also offers a chance for spiritual connection. For patients who can’t attend religious services–and during COVID-19, that’s nearly everyone–Peggy is happy to perform gospel songs and hymns.
Often collaborating with a VITAS chaplain, she puts on an inpatient liturgy for those who request it, giving her a chance to practice the skills she learned in church choir.
How pastoral care supports patients and families >
Playing and singing are just two ways Peggy uses music to connect with and comfort her patients. Depending on the patient’s needs, goals, and level of ability, she may help them write a song, improvise a melody, learn rhythm with percussion, or express their emotions and experiences using music as a medium.
Even when a session is more passive than interactive, Peggy is always assessing the patient’s response and calculating how best to help further:
- Did a song not resonate?
- Is a patient responding poorly to the sound of an instrument?
- Has a lyric struck an emotional chord worth exploring?
Peggy’s melodious voice pairs well with her sharp eye and sensitive ear. She keeps her attention on the patient at the center of the hospice care model.
She also observes and engages with the patient’s caregiver or caregivers, whose tireless work in the patient’s “circle of care” offers useful insight and sometimes warrants specialized care of their own.
“The caregivers are there with the patient all day long. They know her mood intimately, they get excited for her, and sometimes they become tearful as well,” Peggy says. “I think music therapy helps them deal with caregiving, which is very difficult–emotionally, mentally, and physically. The caregivers really engage in it too, singing along and giving encouragement. You can tell that it means a lot to them to see how she’s responding.”
Music Therapy Goes Mainstream
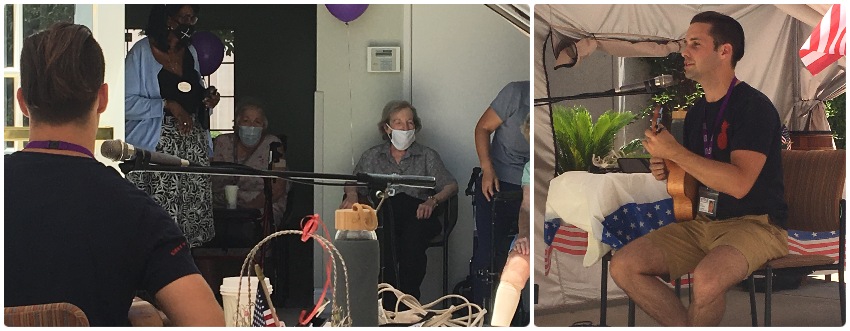
During the COVID-19 pandemic, VITAS music therapists across the United States also have performed concerts for larger groups of residents at nursing homes and other long-term care facilities. These have included musical performances to commemorate important holidays, such as Memorial Day.
Peggy acknowledges that music therapy might seem a little odd to those who have never witnessed a session and may have misgivings about music as a palliative intervention. But over her 18-year career, she’s watched the discipline become increasingly accepted by mainstream professions, and today, she finds it easy to vouch for.
When talking to nurses and clinicians about the benefits of her work, Peggy readily speaks in medical terms and practical impacts. To others, she highlights the spiritual aspects of the therapy, or outlines the specific interventions she performs and how they address a patient’s symptoms.
Words can go a long way in shining a light on “the mystery” of music therapy, but nothing beats witnessing it in action.
“I think what really convinces [skeptics] is when they actually see a music therapy session and how it can help the patient,” Peggy says. “They can’t always put it into words, but they almost always get it.”
Peggy stumbled into music in her early 20s, realizing she had a talent for singing after joining a church choir. The notion of using her talent to care for those who were sick or isolated resonated with her, but she didn’t act on the idea immediately. She finished a bachelor’s degree in vocal performance at Jacksonville University, waiting for some time before deciding to pursue a master’s degree in music therapy.
The wait was worth it.
“I eventually realized that music therapy was my path in life, and hospice was my calling,” Peggy says. “Music therapy is music with a purpose. It may look like I’m having fun, and that’s because I am. I love my job.”

Talking About Hospice
Do you want to start a conversation with your family about hospice?
Download Our Discussion Guide